Assessment of Vocal Nodules
A hoarse voice that persists for more than two to three weeks should be examined. A thorough voice evaluation should include a physician’s examination, preferably by an otolaryngologist (ENT), and a voice evaluation by a speech-language pathologist (SLP) (ASHA, 2011).
Laryngoscopic Evaluation
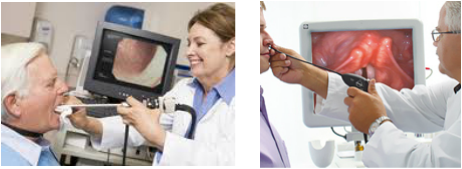
It is the ENT’s task to determine the medical diagnosis, if any, that a person has. This is done through an instrumental examination called laryngoscopy. The purpose of a laryngoscopy is to obtain a detailed picture of laryngeal structure and function. It involves inserting an endoscope, which is a tiny mirror, into the mouth or nose to look at the larynx in general and the vocal folds in particular. The addition of a small camera and light, or stroboscope, may be attached to the endoscope to watch the vocal folds as they move (ASHA, 2011). Endoscopy allows visualization of the vocal folds during phonation and respiration. Examination using a stroboscope provides additional information about the vibratory and closure patterns of the vocal folds (Pedersen & McGlashan, 2000). Through this process a medical diagnosis of vocal nodules can be made.
The following are the different pieces of equipment that can be used to perform the laryngoscopic examination of vocal nodules. Advantages and disadvantages of each method are listed.
The following are the different pieces of equipment that can be used to perform the laryngoscopic examination of vocal nodules. Advantages and disadvantages of each method are listed.
Mirror Laryngoscopy

A small mirror on a handle is placed on the client’s soft palate so that the vocal folds can be seen from above. The client is asked to produce a continuous vowel sound (i.e. /i/) to visualize the vocal folds during motion. This method is easy to administer and cost effective. However, images are small and there is no permanent record of these images. In addition, it does not allow examination of normal speech since the mirror in the mouth prevents the individual from speaking (Williamson, 2008).
Rigid Endoscopy

This instrument is also placed in the mouth towards the back of the throat. This handle, however, has a lens that sends images of the vocal folds to a camera. The vocal folds can only be seen at rest or during phonation of vowel sounds, but the images are much clearer than the images seen with mirror laryngoscopy and they can be saved to a computer and enlarged for viewing (Williamson, 2008).
Flexible Nasendoscopy

A narrow, flexible, fiberoptic cable with a camera attached is inserted into the nose to a position at the back of the throat above the vocal folds. Local anaesthetic nasal spray is usually used to minimize discomfort. The advantage of this technique is that the vocal folds can be viewed during normal speech and singing since there is no instrument in the mouth to prevent this. Images can be saved to a computer for viewing and processing (Williamson, 2008).
Stroboscopy
Since the vocal folds vibrate so quickly, it is not possible to see the individual movements. But with the aid of a stroboscope, which can be fitted to a rigid endoscope or to a flexible nasendoscope, the vibratory cycles of the vocal folds can be viewed as if they have been slowed down or made to stand still. A stroboscope emits flashes of bright light which can be coordinated with the frequency of vibrations (Williamson, 2008).
The following videos show how trans-nasal endoscopy is administered and explain what is seen through this evaluation.
Once the individual has had an ENT examination, speech-language pathology assessment can begin in order to make a voice diagnosis. The SLP needs to take a very detailed case history by asking questions regarding onset and duration of the problem, medical history, description of voice use, and variability throughout the day. The SLP will then evaluate pitch, loudness, and quality of the person’s voice, and will also assess vocal techniques such as breathing and style of voicing. This is done through perceptual and instrumental evaluation. A voice recording is often made, and trial therapy techniques may be used to test their effectiveness at improving the voice (NICD, 1999).
Perceptual Evaluation
The perceptual evaluation involves describing the voice solely by listening to it. Boone states that the perceptual evaluation is important for defining overall therapy goals, helping the patient achieve a target production, and measuring treatment outcome. Throughout the evaluation, the SLP will engage the client in conversation and obtain a detailed case history. Although this may appear as mere “chatting,” the SLP is conducting an informal evaluation of the voice on a principled basis.
Formal perceptual evaluation involves using a protocol to describe and quantify voice difficulty. Areas such as quality, pitch, loudness, resonance, rate, prosody, and aerodynamic measures are assessed (Williamson, 2008). One commonly used protocol is the GRBAS scale, which assesses grade (overall voice abnormality), roughness, breathiness, asthenia (voice weakness), and strain. Another popular protocol, the Buffalo Voice Profile system, rates tone, pitch, loudness, nasal resonance, oral resonance, breath supply, muscles, voice abuse, rate, speech anxiety, speech intelligibility, and provides an overall voice rating (Boone, McFarlane, Von Berg, & Zraick, 2010).
Formal perceptual evaluation involves using a protocol to describe and quantify voice difficulty. Areas such as quality, pitch, loudness, resonance, rate, prosody, and aerodynamic measures are assessed (Williamson, 2008). One commonly used protocol is the GRBAS scale, which assesses grade (overall voice abnormality), roughness, breathiness, asthenia (voice weakness), and strain. Another popular protocol, the Buffalo Voice Profile system, rates tone, pitch, loudness, nasal resonance, oral resonance, breath supply, muscles, voice abuse, rate, speech anxiety, speech intelligibility, and provides an overall voice rating (Boone, McFarlane, Von Berg, & Zraick, 2010).
Instrumental Evaluation
The instrumental evaluation involves using technological instruments to assess the voice. Acoustic analysis is the objective counterpart of the perceptual evaluation. It evaluates many parameters including frequency, intensity, and perturbation, by using instruments that are specifically designed for this purpose. Examples of these instruments are a sound level meter, a spectrogram, or software programs that evaluate several parameters at once, such as KeyPENTAX’s Computerized Speech Lab (CSL) (Williamson, 2008).
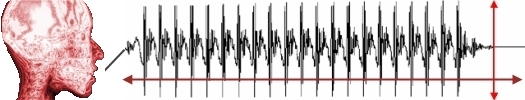
Electroglottograpy (EGG) is another instrumental evaluation technique. It is a non-invasive device issued to estimate vocal fold contact patterns during phonation. Two electrodes are placed on either side of the larynx and a current is passed between them. Vibrations of the folds change the contact area between the electrodes which is registered as changes in resistance. The resulting waveform is termed an electroglottogram and reveals information about vocal fold contact over time. It is used to visualize various types of voice quality (Boone et al., 2010).
Niebudek-Bogusz, Fiszer, Kotylo, & Sliwinska-Kowalska (2006) conducted a study to assess the value of acoustic analysis in diagnosing occupational voice disorders in teachers, which is the profession with the highest risk of developing voice disorders. Subjects included 66 teachers, 35 of whom had voice pathologies such as vocal nodules and 31 subjects with functional dysphonia. Videostroboscopy, the gold standard in diagnosing voice disorders, was used as a reference to compare the results of acoustic analysis. Acoustic analysis was done using the IRIS software to assess areas such as fundamental frequency, jitter, shimmer, and noise to harmonic ratio. Results indicated statistically significant abnormalities in the subjects’ voices. This study shows that acoustic analysis is an effective complement to other forms of voice evaluations. It can be used to diagnose occupational voice disorders and particularity to distinguish between organic and functional dysphonia.
Electroglottograpy (EGG) is another instrumental evaluation technique. It is a non-invasive device issued to estimate vocal fold contact patterns during phonation. Two electrodes are placed on either side of the larynx and a current is passed between them. Vibrations of the folds change the contact area between the electrodes which is registered as changes in resistance. The resulting waveform is termed an electroglottogram and reveals information about vocal fold contact over time. It is used to visualize various types of voice quality (Boone et al., 2010).
Niebudek-Bogusz, Fiszer, Kotylo, & Sliwinska-Kowalska (2006) conducted a study to assess the value of acoustic analysis in diagnosing occupational voice disorders in teachers, which is the profession with the highest risk of developing voice disorders. Subjects included 66 teachers, 35 of whom had voice pathologies such as vocal nodules and 31 subjects with functional dysphonia. Videostroboscopy, the gold standard in diagnosing voice disorders, was used as a reference to compare the results of acoustic analysis. Acoustic analysis was done using the IRIS software to assess areas such as fundamental frequency, jitter, shimmer, and noise to harmonic ratio. Results indicated statistically significant abnormalities in the subjects’ voices. This study shows that acoustic analysis is an effective complement to other forms of voice evaluations. It can be used to diagnose occupational voice disorders and particularity to distinguish between organic and functional dysphonia.